Introduction
In this paper, Anagnostou and colleagues “discuss endpoints used in I-O trials to date and potential optimal endpoints for future early- and late-phase clinical development of I-O therapies”. They establish that classical dose-response patterns are often nonapplicable in the field of immuno-oncology, during the toxicity and response assessment phases in clinical trials. In this paper, they discussed new possible endpoints and methods to obtain clinically relevant data. This is particularly needed when addressing the ongoing development of checkpoint modulators.
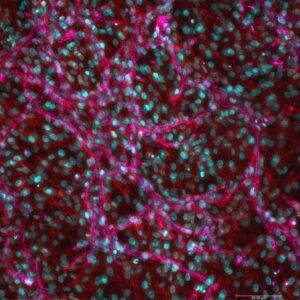
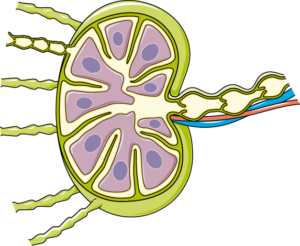
How to culture vascularized & immunocompetent 3D models in a standard Multiwell
Summary
Immuno-oncology (I-O) has required a shift in the established paradigm of toxicity and response assessment in clinical research. The design and interpretation of cancer clinical trials has been primarily driven by conventional toxicity and efficacy patterns observed with chemotherapy and targeted agents, which are insufficient to fully inform clinical trial design and guide therapeutic decisions in I-O. Responses to immune-targeted agents follow nonlinear dose-response and dose-toxicity kinetics mandating the development of novel response evaluation criteria. Biomarker-driven surrogate endpoints may better capture the mechanism of action and biological response to I-O agents and could be incorporated prospectively in early-phase I-O clinical trials. While overall survival remains the gold standard for evaluation of clinical efficacy of I-O agents in late-phase clinical trials, exploration of potential novel surrogate endpoints such as objective response rate and milestone survival is to be encouraged. Patient-reported outcomes should also be assessed to help redefine endpoints for I-O clinical trials and drive more efficient drug development. This paper discusses endpoints used in I-O trials to date and potential optimal endpoints for future early- and late-phase clinical development of I-O therapies.
References
FAQ
The field of immuno-oncology (I-O) has made it necessary to change the established paradigm for assessing toxicity and response in clinical research. The design and interpretation of cancer clinical trials have historically been guided by the conventional patterns of toxicity and efficacy. These patterns are the ones observed with chemotherapy and targeted agents. It has been found that these conventional patterns are not sufficient to fully inform the design of clinical trials for I-O. They also cannot properly guide therapeutic decisions in this specific field. Classical dose-response patterns, which are used in toxicity and response assessment, are often not applicable in immuno-oncology. This has led to a discussion about new possible endpoints and methods to get clinically relevant data.
Responses to agents that are targeted to the immune system are different from conventional chemotherapy. These I-O agents are noted to follow non-linear kinetics for both dose-response and dose-toxicity. This is a key difference from the patterns seen with chemotherapy and other targeted agents. These conventional patterns have historically driven the design of clinical trials. The non-linear nature of immune-targeted agents makes these older assessment methods insufficient. This mandates that new criteria for evaluating responses must be developed. These new evaluation criteria are needed to properly assess the activity of I-O therapies.
For the early-phase clinical development of I-O therapies, different endpoints are being considered. It is suggested that surrogate endpoints driven by biomarkers may be a better option. These types of endpoints might be able to better capture the mechanism of action of the I-O agents. They could also provide a more accurate measure of the biological response to the treatment. It is proposed that these biomarker-driven surrogate endpoints could be incorporated prospectively into the design of early-phase I-O clinical trials. This is part of an effort to find new ways to obtain clinically relevant data, which is needed as new checkpoint modulators are developed.
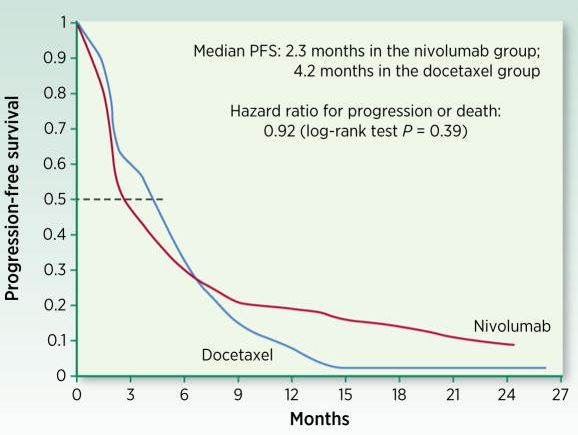
In late-phase clinical trials, overall survival is still considered the gold standard. This endpoint is used for the evaluation of the clinical efficacy of immuno-oncology (I-O) agents. However, the exploration of potential new surrogate endpoints is also encouraged. Examples of these novel surrogate endpoints include the objective response rate. Milestone survival is another endpoint being explored. In addition to these measures, it is also suggested that patient-reported outcomes should be assessed. Including these outcomes could help to redefine the endpoints for I-O clinical trials. This, in turn, could help to drive a more efficient process for drug development.